Originally this was going to be a multi-subject entry, but trying to explain hydroxchloroquine took a
lot more words than I had anticipated, so for today I'm just going to try to tackle this one topic. Tomorrow, other randoms as we wrap up one hell of a week in COVID land.
The Billy Rubin blog staff had a bit of a temper tantrum earlier in the week on the subject of hydroxychloroquine, puzzling some of Billy's Facebook friends as they tried to understand why the innocent question of "why does this not work?" was met with replies that, to put it bluntly,
were raving. The outbreak is bringing out the best and worst in Dr. Rubin, and among his worst traits is a lack of patience with what he would describe as "bad medicine." In professional circles, for the most part, he works very hard not to lose patience. On Facebook, though, he ranted a little without explaining himself properly. As a consequence, he's now a little embarrassed, and consequently is referring to himself in third person to make it look like it's someone else entirely.
Here is a more sober explanation of the problem. It's a
long explanation. But let me note that absolutely nothing has changed my conviction that what has transpired on the subject of hydroxychloroquine is, from a professional standpoint, shameful. "Shame" is a strong word to use in the realm of medicine; we don't like throwing feces balls at each other like enraged chimpanzees. But it's unfortunately the right word, and unmasks a collective philosophical problem in medicine that irks all members of the Billy Rubin Blog staff.
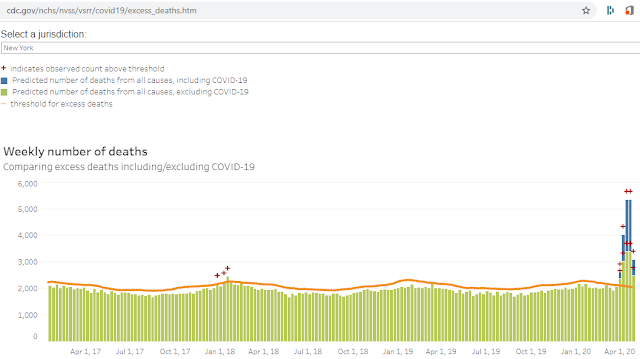
Let's start at the beginning, all the way back to just over two whole months ago, in Wuhan, China, in the early days of the outbreak. As
we now see in New York, the healthcare system in Wuhan was overwhelmed, and the doctors there lacked any known, specific therapy for an unknown virus that looked one hell of a lot like its genetic cousin SARS (what we know now but didn't then is that COVID is significantly less lethal than SARS, and for which the world should be breathing a deep sigh of relief). The doctors there, in a valiant but ultimately uncoordinated attempt at doing
something, started trying out whatever they had in their arsenal that could be reasonably justified on biological grounds, and this included a variety of drugs used in treating
other viral infections. (Side note: I'm no expert on the subject of the infrastructure of Chinese medicine, but based on reading years of medical papers out of China, and doing a brief sojourn to Beijing, Xi'an, and Luoyang a few years back, I'm reasonably confident that Chinese medicine in the urban areas is effectively indistinguishable from the West. The idea that China is third- or second-world in its living standards is well out of date at this point.)
The
discussion of these drugs got a glancing mention in the report on the early outbreak issued by the WHO and Chinese CDC (see bottom of page 32 if interested). Because everyone was trying to play nice together, the language is careful to avoid judgement, and basically says, "well, doctors tried this stuff." The drugs included the following:
chloroquine: an antimalarial--
not an antiviral, more on that in a second;
lopinavir/ritonavir: a drug used in treating HIV known as a
protease inhibitor, more on that in a second, too;
alpha interferon: an old drug used mainly for treating Hep C until new drugs came along, now almost never used in the US;
ribavirin: an old drug used now mainly for two very different viruses, a respiratory virus called RSV, and a hemorrhagic fever virus called Lassa Fever
The paragraph ends with a nod to traditional Chinese medicines, where it was noted "the effects [of which] must be fully evaluated." No snark about Chinese medicines coming from me on this; the problem isn't the medicine itself,
only how such compounds get evaluated so that we can know what works and what doesn't. And the same could be said of these "well, we tried this stuff" drugs. But the rationale behind using some of these drugs is, in my opinion, very thin.
Let's take the lopinavir/ritonavir example before getting to chloroquine and hydroxychloroquine. As I said, lopinavir is an HIV protease
inhibitor. What's a protease? Well, when HIV reproduces, it starts out as this long strand of nucleic acid; the HIV strand then uses the body's own cellular machinery to "translate" that strand into one huge combination of
all the proteins used in making an HIV particle. It would look like an Ikea set
with every single piece of the furniture, from the big pieces to the individual screws, taped together. The function of the protease is to
cut those pieces of tape to allow for assembly. Thus a protease
inhibitor keeps everything glommed up together so that it can't be assembled. Protease inhibitors remain one of the mainstay drugs in treating HIV, though lopinavir is now a third-line drug in the US and Europe owing to very real and unpleasant side effects--side effects that could be lethal in a sick person.
Anyway, coronaviruses like COVID
have their own proteases, so the basic reasoning was, "well, since both viruses have proteases, maybe it'll work." It wasn't that shot-in-the-dark, though: despite the fact that HIV is a
very different virus and is far away from COVID on the evolutionary tree, the reasoning
was based in scientific research, as
this paper notes that lopinavir appeared promising as an anti-SARS drug as long ago as 2005. Every drug used by the doctors in Wuhan follows a similar rationale. They did their homework, for sure--and that they did so in the midst of being overrun by a plague that felled members of their own ranks, including a number of
people who not only braved the virus but also told truth to power, should earn our eternal thanks, regardless of where we find ourselves on the ideological divide with respect to our governments.
Chloroquine
is a drug whose formal development goes way back 1945, but its roots date much further back to the
early seventeenth century, when European empires began their systematic program for extracting resources from the tropics in earnest. The
earliest Western observations came from observing the medicinal properties of preparations from the bark of the
Cinchona tree in the Andean region of South America. The Cinchona gave us quinine, the critical ingredient in the original Gin & Tonic, which in addition to being a delight to drink, provided legitimate protection against malaria. From there, the massively oversimplified story of chloroquine requires a fast forward to the early 19th century, when the foundations of modern medicine were being laid by the development, of all things, of the modern dye industry, because they eventually begat German biochemical and pharmaceutical companies like IG Farben. (If you're puzzled by seeing a reference to dye makers, the link is that 19th-century scientists discovered that some dyes like methylene blue had antimalarial properties, which led to further research. In fact, the story of the link between the dye industry and infectious disease is a pretty fascinating one, as
the story of the development of Bactrim--still ubiquitous in modern medicine--cannot be told without explaining its origins in dye research and development. But we're getting far afield, and we still haven't gotten to the meat of this post.)
Anyway,
chloroquine was the most promising of the antimalarials that came out of the mid-20th century research, and its mass production led to the first reliable industrial treatment of the disease. At the same time, physicians who were trying to understand the biological process of inflammation (which, one hundred years later, we're
still trying to understand) noted that part of chloroquine's effectiveness seemed to reside not only in how it killed the malaria parasite, but also that it seemed to tamp down the human (or "host," in sciencespeak) inflammatory response. That is, it appeared that part of malaria's lethality was not only directly from the parasite, but also from the exaggerated host immune/inflammatory response, and chloroquine seemed in part to work by pulling the reins on inflammation. Which made people wonder whether it might be useful in
other diseases where the body had an exaggerated immune response, but not in the setting of malaria. (Spoiler alert:
it was.)
The upside was that chloroquine could save you from malaria; the downside was that it wasn't an entirely benign drug in its own right. Tinkering with the drug, chemists added a "hydroxyl" group onto chloroquine (which is to say, an oxygen atom attached to a hydrogen atom), and thus was born hydroxychloroquine. It was one of many different variants that was studied at the time and was found to be as effective against malaria as chloroquine, but with a much more favorable safety profile. This is the bread and butter of what drug companies do, and it's worth noting that chemists in these companies create
hundreds of compounds, all slightly different, and run preliminary tests to identify the most promising compounds that might make it to a human trial. Hydroxychloroquine was just one of these hundreds of compounds at the start of the process, and many more drugs fail to get to a drug trial than those that don't--
and most of those that make it
to a drug trial end up failing as well.
Malaria falls out of this drama by the late 20th century owing to the fact that malaria got wise and developed resistance to chloroquine and hydroxychloroquine, such that
there are now few malaria-endemic areas on earth where the drugs still work. Thus, by the time we arrive in the pre-COVID world of early December 2019, hydroxychloroquine's use mainly resided in its anti-inflammatory properties. And the principal diseases of inflammation where they have been found to be most effective have been in
lupus and (to a more limited extent) in
rheumatoid arthritis.
Newer agents have begun to replace hydroxychloroquine, but particularly in lupus, hydroxychloroquine is still commonly used. Which means lupus patients need those drugs to be stockpiled for their use.
The use of chloroquine and hydroxychloroquine in the treatment of
viral infections
dates back to at least the early 1980s, again as virologists tinkered around labs seeing what drugs worked and what didn't against some pet virus. And chloroquine/hydroxychloroquine's record against viruses in the laboratory is pretty good. Poke around Pubmed for awhile and you can see promising results against
influenza,
Hepatitis C,
HIV, and, of course,
SARS--a virus that can be thought of as the raging beast relative of COVID, the Trump to COVID's George W Bush, as both are deadly, but one significantly more so. Since January,
virologists were able to see the same antiviral effect against COVID, as well. But this is all "in vitro" data, which is to say, those experiments just looked at what the drug did with the virus on the battlefield of a few cells in a petri dish.
That was the background behind hydroxychloroquine's star turn on the COVID stage. But did it work? The most intellectually pure scientific answer is "we don't know." The most
likely answer, in the opinion of the Billy Rubin Blog Editorial Staff, is "nope."
The original
clinical evidence supporting hydroxychloroquine came from a study
found here in the International Journal of Antimicrobial Agents. (Note: this study may be amended, or even withdrawn, but the point is where it moved the needle with respect to how it influenced the medical community, and ultimately, Donald Trump, in March 2020. Thus, post-hoc changes to the article matter little.) The study evaluated 42 patients: 26 got hydroxychloroquine, and 16 did not.
Before we get to just how bad a study it is, let's ponder that sample size for a second. And to get context for that, there needs to be a discussion about case fatality rates.
There is
now spirited debate about just how lethal COVID is--is it one percent, or four, or zero-point-five? For my part, I'm going with two general numbers: the
overall case fatality of everyone who gets infected is about one in two hundred (or 0.66 percent)--but this is only a rough estimate because we don't know how many people there who have very mild symptoms, or no symptoms at all, since they don't get tested. By contrast, the case fatality rate of people who develop obvious symptoms of illness is somewhere around
four or maybe
five in one hundred. Overall I think this is a sideshow except for the epidemiologists who need to figure out things like herd immunity in their modeling of just how bad this epidemic is going to get.
But from a
clinician's standpoint, the latter number (ie CFR of 4-5%) is far more important, because what we really want to know when using a drug is: if I use this on someone, how likely am I to save a life? And to do that you have to know how many people would die from doing nothing at all. Hopefully everyone out there can see that, if you have a disease in which four people out of one hundred die, then recruiting 42 patients is not going to tell you what you need with any confidence, as all 42 could simply survive by chance. So that's strike one against the study--and it's a
big strike, so kinda worth strike two as well.
But there can be clever ways to use a small sample size and get
surrogate data to tell you whether doing a full, count-em-up clinical trial to look directly at mortality is worth it. In this case, the surrogate marker is the amount of virus people have in their bodies. This was the finding that got everyone's attention, and it was mainly due to this picture:
It
purports to show that those who got hydroxychloroquine (the red line) had a much faster decline in their viral loads than those who didn't--and from that, the conclusion was that we should try this out clinically. The problem, or at least one among many,
as extensively outlined in this extremely well-written blog by David Gorski, a surgical oncologist with a PhD and who writes often on clinical trials and the statistics that underlie the work, is that even this scant data is cherry-picked, as (for starters) patients who were moved to the Intensive Care Unit--which is to say,
the sickest ones--got left
out of the hydroxychloroquine group. This borders on scientific malpractice, and is a rookie error of clinical trial design. In fact, we don't even expect rookies to make mistakes like this.
But what happened in the medical world, even before Donald Trump came along and made everything much worse, was that only the punch line got repeated (hydroxychloroquine works!), and nobody took a direct look at the data to see just how shoddy it was. That's understandable in the layperson world, but for doctors who are trying out untested and potentially dangerous medications in critically ill people, it's the worst kind of laziness. Doctors were prescribing this drug (or, appallingly,
hoarding it for their own use) because they read somewhere or heard from someone who spoke to someone who read something that "maybe this works." Well,
maybe it does work. But
maybe ozone therapy works for Ebola, too. (Hint: it doesn't, really.)
Hydroxychloroquine thus became the great hearsay drug in the early hours of the COVID epidemic. It had no proof, a vaguely plausible justification for its use, and ready availability. But by mid-March, there was still very much no there, there.
Then Trump's tweet came on March 21. I won't say much about this chapter of the saga other than to note that it should be self-evident that there is a high inverse correlation between
any pronouncement Donald Trump makes and its truth value. Thus, the fact that he touted the drug (along with a second drug we don't have time to go into, azithromycin) could be reasonably regarded
a priori as clinically useless, or at least wildly overblown, simply by dint of the fact that Trump endorsed it.
Meanwhile, in
Fantasyland, tales
from a "simple, country doctor" were filling the airwaves of the magical hydroxychloroquine elixir. The doctor in question is one Vladimir Zelenko, who noted that he was "seeing tremendous results" in patients using hydroxychloroquine, azithromycin, and zinc. How could such a simple country doctor outwit such heavyweights as
Anthony Fauci, who seemed to remain stubbornly skeptical of hydroxychloroquine when doctors like Zelenko could see its obvious promise? Was Fauci secretly part of the Deep State trying to take down Trump by making things
worse and
withholding lifesaving, and readily available, drugs?
The answer to these questions are simple:
Zelenko's simple. He is, like his President who took to the Twitterverse in enthusiastic endorsement, a living, breathing,
perfect example of the Dunning-Kruger effect. He is so hopelessly in over his head that he has no mental tools to understand just how in over his head he really is. Maybe--
maybe--if COVID were as lethal as Ebola, simple country doctors could see for themselves if a drug worked without having to resort to clinical trials, or troublesome issues like placebo controls and informed consent, or confidence intervals and power calculations. But with this virus? Not so much. You need the machinery of modern medicine, and the research tools that took two centuries to develop, to really know whether you're making an impact. But he has no clue
that he has no clue. And so can be said for the followers of Donald Trump, who have been remarkably resistant to grasp his obvious buffoonery, despite it being on daily display over the past month. It's quite impressive, really. Denial is a powerful thing.
But let's end not on the cartoonish stupidity of the President and his Republican enablers, let's turn back to what under normal circumstances would a be solid place to find information, for even they can make the occasional slip-up. And this week,
a piece in the New York Times described a
new trial on hydroxychloroquine
in which the results were favorable. It's certainly a better study than the one mentioned above, though that's a pretty low hurdle. But it's not
substantially better: it once again enrolled too small a cohort to look directly at mortality, so it relies on surrogate data that make it hard to know whether the benefit is real or an optical illusion; the patient population studied never got very sick, making its relevance in saving lives of unclear significance; and people did suspiciously well in this cohort, potentially suggesting some unseen bias that shaped the numbers. Everyone in my division took a look at the paper: the reaction was swift, and it wasn't anywhere near as favorable as the warm coverage in the article.
The study hasn't been peer reviewed, where these and other troubling issues would be addressed. Perhaps upon peer review, the study might not even be published because it is found to be wanting. The question, then, is why did
NYT pick it up? At the Billy Rubin Blog, we're scratching our heads on that one, because the publication of this article just made it harder for every ID doctor everywhere to try to do their jobs, in no small part because we have to continuously explain to stressed and worried families at length why these studies aren't really very good, and that these drugs come with side effects that might actually
end their loved ones life, not save it. This blog entry, despite running to thousands of words, hasn't even taken a shot at explaining a heart-stopping effect called the
long QT syndrome, which is almost certainly hydroxychloroquine's most deadly acute effect, and is even worse when used in conjunction with azithromycin, and which I've seen once already in a COVID patient.
Ultimately, there's an old saying in medicine that encapsulates the skepticism that we should be applying toward hydroxychloroquine's boosters, whether those boosters are motivated by naked partisan political considerations (which is to say, Trump, who wants this to go away for narrowly selfish reasons), or by a look-we're-trying-to-do-everything-we-can motivation (doctors who feel they just can't stand around and do
nothing). The saying is
really old, so old that it comes from a different language, and a different epoch, entirely. The language is Latin, and the saying is
primum non nocere. It means, "first, do no harm," and is a caution to physicians who panic in the midst of an outbreak by trying to throw everything at the wall and seeing what sticks.
With a four percent case fatal virus, you cannot see what sticks unless you do a clinical trial. With a drug like hydroxychloroquine, off-the-shelf use is a recipe for killing not only
one patient--the COVID patient receiving the drug--but possibly a
second as well. That person is the lupus patient who has been denied their drug. Because soon, stockpiles of hydroxychloroquine, like the ventilators that are crucial to the survival of the sickest COVID patients, will have dried up.
Among the many lessons that the West African Ebola outbreak had to teach was that physicians shouldn't lose their collective clinical head in a disaster. We should take a page from Douglas Adams, and conduct ourselves by the motto
don't panic. We should treat patients by what we
know works, not what we
hope works, because we're probably going to
kill somebody if we practice medicine that way, and we're no better than the
Quacks of Old London in the 1600s. We do what we can, and in the meantime, we (urgently) do well-designed, adequately-powered clinical trials to learn what works and what doesn't. That includes a trial of hydroxychloroquine! But without doing good science, we're
the same as doctors during the bubonic plague, or at least not as good as we could and should be.
There were no good clinical trials that came out of the West African Ebola outbreak.
That failure was enough to get a group of experts together to work with US, European, and African countries so that they were more prepared to do quality clinical trials when the next Ebola outbreak came. Thus, it came to pass, that good clinical trials were conducted in a much more challenging Ebola outbreak in the Congo, so that
now we have two therapies that dramatically reduce the mortality from Ebola.
There is no reason why we cannot do such research right now, and adjust our practices as fast as humanly possible, in the midst of
this outbreak, especially as it may not be over anytime soon.
--Billy